How Denmark, Sweden and Norway have fought against Omicron and what Australia must do to catch up
With other countries either suspending or abolishing their Covid restrictions, there is a key factor preventing Australia from doing the same.
After more than two years of having our lives dictated by the Covid pandemic, many are no doubt looking forward to the day when the pandemic finally disappears.
For a number of Scandinavian and European countries, this may be their reality.
In the lead, Denmark removed all Covid restrictions on 1 February, Norway also removed the majority of the restrictions and Sweden followed after 9 February.
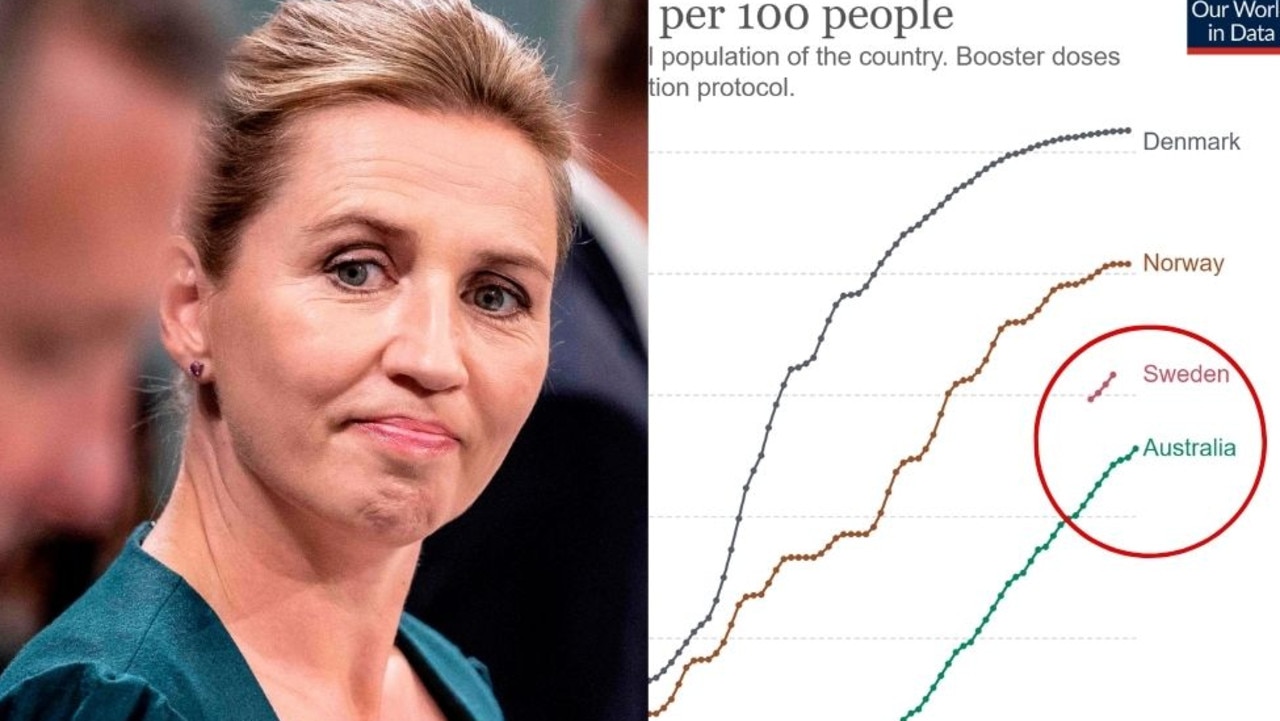
When looking at when Australian authorities can adopt similar rules as our Scandinavian counterparts, Deakin University’s chair of epidemiology, Professor Catherine Bennett says there is one key area where Australia is lacking: booster doses.
As of February 9, just under 9.2 million Australians over the age of 16 had received more than two doses of the vaccine, which is about 35 per cent of Australia’s total population.
Conversely, more than 61 percent of Denmark’s population has received booster shots, 50 percent of Norwegians and 42 percent of Swedes also triple injured.
“Although we have the highest numbers overall for primary causes, compared to the three countries, we have the lowest booster rate because our first course was launched later,” says Professor Bennett.
“It seems to me that the effect of the booster further reduces the risk of both Omicron infection and the translation into serious illness.”
Denmark: Where Covid is no longer “socially critical”
While Denmark removed all Covid restrictions (for the second time) when the country experienced its largest wave of cases – registering more than 41,000 cases on 1 February – the health authorities believed that declining proportions in need of intensive care were a decisive factor in easing the restrictions.
Despite this, the move received harsh criticism from Tedro’s Adhanom Ghebreyesus, Director General of the World Health Organization.
“We are concerned that a story has gained ground in some countries that due to vaccines and due to Omicron’s high transmission capacity and lower severity, it is no longer possible and necessary to prevent transmission,” he said two days after Denmark removed the restrictions.
“Nothing could be further from the truth.”
But when he spoke to AFP, the prominent Danish epidemiologist Dr Lone Simonsen credited Denmark’s high booster rate and its ability to declassify Covid as a “socially critical disease”.
“We have an extremely high coverage of adults vaccinated with three doses,” says Dr. Simonsen.
“As Omicron is not a serious disease for those vaccinated, we believe it is reasonable to lift the restrictions.”
Norwegian Prime Minister Jonas Gahr Stoere said a similar thing when he removed the limits for visits to the household, mandatory rules for working from home and gave restaurants the green light to serve alcohol after 23:00.
“Although many more people become infected, fewer are hospitalized,” he said.
“We are well protected by vaccines. This means that we can facilitate many measures even when the infections increase rapidly.”
How does Aus compare to hospital stays?
When measuring the current state of Covid in Denmark, Norway and Sweden, Australia seems to be unimaginably leading in figures for hospital stays. Although the difference in population makes a difference, Australia has registered higher ICU numbers. But Australia’s hospital admissions have been steadily declining since February and Dr Bennett believes this will decrease as booster levels rise.
According to the latest figures, Australia with a population of 25.69 million registered 3586 hospital admissions, with 272 patients in the intensive care unit on 9 February.
Sweden with about half of Australia’s population (10.35 million) registered 2089 hospitalizations and 113 cases in the intensive care unit on 7 February.
But one-fifth of Australia’s population, Denmark’s 5.83 million inhabitants, registered 1,152 hospital admissions with only 30 people in need of intensive care.
Norway reports a population similar to Denmark (5.37 million) and has 251 Covid patients treated in hospitals (January 30), with 45 critical cases in the intensive care unit.
Overall, however, the head of Monach University’s epidemiological modeling unit, Professor James Trauer, said that although elective procedures have been affected and Australia’s hospital system has been exposed to a great deal of stress, it never reached the point of “overwhelming” during the pandemic.
“There has been a lot of strain on the health system and but I think we have not seen what has been seen abroad, especially in places like Delhi, Malaysia, Indonesia and Nepal.”
“We have not seen that kind of total overwhelming where people do not get the treatment they need or can not access oxygen.”
But in order for Australia to be able to reduce the number of hospital stays, Professor Trauer said that focus must be placed on increasing booster doses “in older populations”.
“I do not think there has been enough focus on vaccine coverage in older age groups,” he said.
“Since we have had the pediatric launch, we have not had things as targets for the coverage we want to see with doses in older populations.”
What about Australia?
While Australia may not be in a position to remove all of our restrictions, Dr Bennett stresses that we are in a “fundamentally different place” with Covid and will go to a point where “quite a few of us do not think of Covid”.
But she admits that the rise of Omicron has “pushed us even further along this transition path”.
“It has moved people to get used to numbers that were a little higher and that made us live with a virus and we now see it even in WA,” she said.
“I think when the last group of people come on board and admit that we can not control this, it will make things like internal borders a little easier.”
In the end, Prof Bennett predicts that Covid will gradually become less prominent in the lives and minds of Australians, unless a more virulent and contagious variant emerges. While she believes that “we have moved on from similar deadlocks”, she says that things like “reintroducing density limits, mask recommendations and using RATs to screen” can be turned up or down if cases increase rapidly, especially during the colder months where the virus can be spread more easily.
“Having these backups ready and knowing what to expect is not about waiting or watching out for it,” she said, “it’s about not being able to think about it because we know what to do if it should happen.
“It’s about being ready rather than being afraid.”